Breath odour is the presence of odorous volatile organic compounds in the breath of individuals. It is a widespread problem, as it affects a high percentage of the adult population; 30% of the global population suffers from chronic oral malodour and 74% considers it an issue.[1] Breath odour has strong social implications for the sufferer and it significantly affects normal social interactions.
Breath odour can have physiological or pathological causes of intra- or extra-oral origin (Fig. 1). Physiological odour includes morning breath, which is transient and related to low salivary flow during the night. Other lifestyle factors can influence it too, such as smoking, as well as the consumption of alcohol or odoriferous foods and drinks (garlic, onion and cabbage, among others). These are fairly common reasons for concern in the adult population, but can easily be rectified by modification of beverages and foods consumed, toothbrushing, mouthrinses and tongue cleaning. Pathological malodour, however, is more challenging to treat. Extra-oral breath odour can arise from respiratory, gastrointestinal or metabolic issues, which cannot be addressed by oral hygiene, as these do not originate from the mouth.[2–4]
Most cases, however, originate from the oral cavity. Breath odour from intra-oral causes arises from volatile sulphur and organic compounds (VSCs and VOCs, respectively) formed as a result of the degradation of organic substrates by anaerobic bacteria on the dorsum of the tongue, particularly at the back of it.[5, 6] It can also result from gingivitis and periodontitis, and their combination with tongue bacteria. However, in individuals with good oral hygiene and gingival health, the main cause is the bacteria on the tongue (Fig. 2a).[4] Breath odour is generally assessed by organoleptic score, which is determined by a trained odour judge, who measures the strength of target odours and expresses the value according to a predefined scale from 0 (no odour) to 5 (strong malodour).
A niche for bacterial biofilms
The tongue has a very complex and rough surface structure covered with flexible papillae (Fig. 2b). Those papillae vary in shape, size and distribution pattern and give the tongue a surface with numerous crypts and fissures.[7, 8] This constitutes a perfect microbial niche for anaerobic bacteria to thrive and form thick biofilms largely undisturbed. Bacteria can degrade a complex mixture of amino acids and proteins from numerous origins (diet, debris, cells) with their complex enzymatic machinery. Particularly the degradation of amino acids, such as cysteine and methionine, produces VSCs with a very high odour power.[9] The bacterial density on the tongue surface has been related to the degree of breath odour.[10–12] For example, individuals with noticeable breath odour (above 2.5 in the 5-point organoleptic scale) have more than 1 × 108 bacterial colony-forming units per sqcm of the tongue, while individuals with lower organoleptic scores harbour lower bacterial numbers (approximately 1 × 107).[12] Therefore, in order to reduce breath odour in patients, the tongue bacterial density must be reduced and kept at low levels.
Treatment of oral malodour
There are numerous over-the-counter products for oral malodour and these can be divided into chemical and mechanical treatments. Chemical treatments are mostly mouthrinses specifically developed for oral malodour, containing a combination of antimicrobials and metal ions. Commonly used antimicrobials are chlorhexidine and cetylpyridinium chloride (CPC), which have a strong effect in killing bacteria. Metal ions, such as zinc, bind to sulphur compounds and form insoluble complexes (zinc sulphide) that are not volatile and are therefore non-odoriferous.[10, 13–16] Another category of mouthrinses for malodour contains chlorine dioxide, which neutralises the sulphur gases and oxidises VSCs, while the chlorite anions act as an antibacterial compound.[17] While mouthrinses have the potential to be very effective owing to their antibacterial and oral malodour-masking properties, they rarely provide a long-lasting result. They are effective for a few hours, but they have little effect on the tongue bacterial density.[18, 10] A possible cause of this limited effect on the tongue is that the active components of mouthrinses cannot reach the odour-producing bacteria. Biofilms that produce volatile gases are mostly located deep between the tongue papillae (Fig. 2c), where mixing and diffusion of active ingredients are difficult owing to the small papillary spaces, the viscosity of salivary molecules and the low permeability of biofilms.
embedImagecenter("Imagecenter_2_2237",2237,"small");
Guidelines for the treatment of oral malodour by dental professionals emphasise the need for tongue cleaning using scrapers or brushes. Clinical studies have shown that the use of mechanical methods reduces the tongue coating.[10–21] However, the effect on malodour is very short lived,[19] which is probably due to the reduction of the bacterial nutrients present in the tongue coating rather than the reduction of the bacterial density itself.[22] The limited amount of bacterial removal from the tongue’s complex surface is due to the difficulty in reaching the biofilm between the tongue papillae. Moreover, as the tongue tissue is very flexible, the use of tongue scrapers could flatten the papillae, trapping the bacterial biofilm underneath and not removing it.
Combined approach for all-day fresh breath
The use of mouthrinses in combination with mechanical intervention could help the active ingredients penetrate deeper into the biofilm than when used alone, while simultaneously reducing the tongue coating and bacterial density. The combined approach of chemical and mechanical intervention could have a synergistic effect on oral malodour to deliver full-day fresh breath, as has been shown in recent studies.[23, 20] In a recent clinical investigation, we showed that the combined use of a newly designed sonic tongue brush with an antimicrobial spray delivered a significantly superior reduction in breath odour than did the individual treatments.
Philips Oral Healthcare has recently developed and launched a new sonic powered tongue brush and antibacterial spray combination, Sonicare TongueCare+. The brush has been designed to penetrate between the tongue papillae and to provide thorough mechanical biofilm removal. Bristle dimensions and stiffness parameters were optimised based on analysis of the human tongue. The brush head consists of 240 flexible elastomer MicroBristles mounted on to a Sonicare power toothbrush handle, with 31,000 vibrations per minute to help break up any tongue coating and sweep away debris and bacteria (Fig. 3).
TongueCare+ brush is used in combination with the BreathRx antimicrobial tongue spray (Philips), which contains antimicrobial agents, such as CPC and zinc. In the first proof of principle clinical investigation of this technology, it was shown that the organoleptic score and the tongue bacterial density can be significantly reduced with a single use of TongueCare+ with BreathRx, measured up to 6 hours (Figs. 4a & b). This combined treatment reduces breath odour significantly more than using TongueCare+ alone or BreathRx alone, supporting the idea that a combined approach is likely more effective. Moreover, TongueCare+ has been shown to significantly decrease the tongue bacterial density, which is kept low for up to at least 6 hours, indicating that the root cause of breath odour is addressed with this approach. This, this combination provides a more effective and long-lasting treatment option for people suffering from breath odour.
Possible oral health implications
Overall, it is of key importance to integrate tongue cleaning into the oral hygiene routine in order to have fresh breath all day. Additionally, it has been suggested that the tongue can act as a reservoir of periodontal pathogens for the rest of the mouth,[24, 25] which could colonise other areas and have an impact on oral health in general. Moreover, several studies have shown that VSCs, such as hydrogen sulphide and methanethiol, are toxic to periodontal tissue even when present in very low concentrations, so it has been hypothesised that they can contribute to the progression of gingival diseases.[26] Therefore, maintaining a good tongue cleaning routine could have far-reaching implications.
Editorial note: A list of references is available from the publisher.
Conflict of interest: Dr Paola Gomez-Pereira is a senior scientist at Philips in Cambridge in the UK.
Breath odour is the presence of odorous volatile organic compounds in the breath of individuals. It is a widespread problem, as it affects a high percentage...
LONDON, England: Driven by the NHS dental crisis, an increasing number of UK patients seeking cheaper dental work overseas are encountering unexpected ...
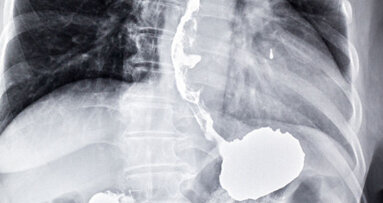
LONDON, UK: An international team of researchers has developed a breath test that could help doctors diagnose the early signs of oesophageal and gastric ...
LONDON, UK/AMSTERDAM, Netherlands: A test that measures the levels of five chemicals in the breath has shown promising results for the detection of cancers ...
BRISTOL, UK: Researchers at the University of Bristol have developed a new technology that could increase protection against anti-bacterial and anti-fungal ...
SHEFFIELD, UK: In Western countries like the UK, between 10 and 20 per cent of adolescents undergo orthodontic measures in some form. A recent meta-analysis...
DUBLIN, Ireland: An unregulated use of fortified high-sugar food supplements is causing untold damage to the oral health of thousands of nursing home ...
WAALWIJK, Netherlands: For more than 35 years, the treatment systems developed by Myofunctional Research Co. (MRC) have helped practitioners around the ...
LONDON – The General Dental Council (GDC), the regulatory body for dental professionals in the UK, has suspended a dentist for professional misconduct...
BRISTOL, UK: The University of the West of England (UWE) in Bristol has drawn attention to an unusual course run at its Centre for Research in Biosciences. ...
Live webinar
Wed. 3 June 2026
6:00 pm UTC (London)
Live webinar
Thu. 4 June 2026
7:00 pm UTC (London)
Live webinar
Mon. 8 June 2026
5:00 pm UTC (London)
Live webinar
Mon. 8 June 2026
6:00 pm UTC (London)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
7:00 pm UTC (London)
Live webinar
Wed. 10 June 2026
4:00 pm UTC (London)
Live webinar
Wed. 10 June 2026
7:00 pm UTC (London)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East







































To post a reply please login or register