LONDON, UK/AMSTERDAM, Netherlands: A test that measures the levels of five chemicals in the breath has shown promising results for the detection of cancers of the oesophagus and stomach in a large patient trial. The new research, involving more than 300 patients, found that the test could diagnose cancer with an overall accuracy of 85 per cent.
Together, stomach and oesophageal cancer account for around 1.4 million new cancer diagnoses each year worldwide, according to the Cancer Today magazine. Both tend to be diagnosed late, because the symptoms are ambiguous; consequently, the five-year survival rate for these two types of cancer is only 15 per cent.
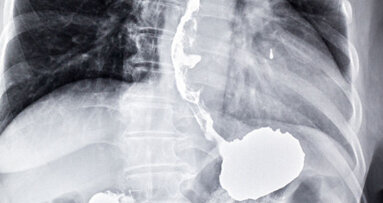
At present, the only way to diagnose oesophageal cancer or stomach cancer is with endoscopy. This method is expensive, invasive and has some risk of complications. “A breath test could be used as a non-invasive, first-line test to reduce the number of unnecessary endoscopies. In the longer term this could also mean earlier diagnosis and treatment, and better survival,” said Dr Sheraz Markar, a National Institute for Health Research Clinical Trials Fellow from Imperial College London, at the 2017 European Cancer Congress, recently held in Amsterdam.
The trial was based on the results of previous research that suggested differences in the levels of specific chemicals—butyric, pentanoic and hexanoic acids, butanal and decanal—between patients with stomach or oesophageal cancer and patients with upper gastrointestinal symptoms without cancer. The new research aimed to test whether this chemical signature that seemed to typify cancer could be the basis of a diagnostic test.
In the study, the research team collected breath samples from 335 people at St Mary’s Hospital, Imperial College Healthcare NHS Trust; University College Hospital; and the Royal Marsden Hospital, all in London. Of these, 163 had been diagnosed with stomach or oesophageal cancer and 172 showed no evidence of cancer during examination via endoscopy.
All the samples were analysed with a technique called selected-ion flow-tube mass spectrometry, which is able to accurately measure small amounts of different chemicals in mixtures of gases such as breath. The researchers measured the levels of the five chemicals in each sample to see which ones matched the chemical signature that indicated cancer.
The results showed that the test was 85 per cent accurate overall, with a sensitivity of 80 per cent and a specificity of 81 per cent. This means that the breath test was good both at picking up those who had cancer (sensitivity) and at correctly identifying who did not have cancer (specificity).
Markar said: “Because cancer cells are different to healthy ones, they produce a different mixture of chemicals. This study suggests that we may be able detect these differences and use a breath test to indicate which patients are likely to have cancer of the oesophagus and stomach, and which do not. However, these findings must be validated in a larger sample of patients before the test could be used in the clinic.”
Over the next three years, the researchers will continue with a larger trial, using the test on patients who have undergone an endoscopy for gastrointestinal symptoms, but have not yet been diagnosed with cancer. This will assess the ability of the test to identify cases within a group that is likely to contain only a small percentage of cancers.
The team is also working on breath tests for other types of cancer, such as colorectal and pancreatic cancer, which could be used as first-line tests in general practice surgeries.
The study, conducted in collaboration with Karolinska Institutet in Sweden and University College London in the UK, was presented at the 2017 European Cancer Congress.
Tags:
LONDON, UK: An international team of researchers has developed a breath test that could help doctors diagnose the early signs of oesophageal and gastric ...
BIRMINGHAM, England: Diabetes is one of the most common chronic conditions in Europe and is strongly associated with periodontitis. An estimated one in ...
BRISTOL, UK: The University of the West of England (UWE) in Bristol has drawn attention to an unusual course run at its Centre for Research in Biosciences. ...
LONDON, UK/ATLANTA, USA: Although the death rate from cancer in general has declined steadily over the past two decades, the latest statistics published by ...
LONDON, UK: Factors such as glucose metabolism, nutrition, oxidative stress and ageing drive periodontal progression. However, current periodontal ...
Breath odour is the presence of odorous volatile organic compounds in the breath of individuals. It is a widespread problem, as it affects a high percentage...
Breath odour is the presence of odorous volatile organic compounds in the breath of individuals. It is a widespread problem, as it affects a high percentage...
LONDON, UK: Seeking to improve oral cancer detection and treatment, researchers from Queen Mary University of London have developed the first polymerase ...
YORK, UK: Fear of the dentist is something some people suffer from more than others. With multiple reasons for dental anxiety and its effects, there is ...
EDINBURGH, UK: A study by researchers at the University of Edinburgh has shown that a natural chemical related to those found in liquorice root could help ...
Live webinar
Wed. 3 June 2026
6:00 pm UTC (London)
Live webinar
Thu. 4 June 2026
7:00 pm UTC (London)
Live webinar
Mon. 8 June 2026
5:00 pm UTC (London)
Live webinar
Mon. 8 June 2026
6:00 pm UTC (London)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
7:00 pm UTC (London)
Live webinar
Wed. 10 June 2026
4:00 pm UTC (London)
Live webinar
Wed. 10 June 2026
7:00 pm UTC (London)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East






































To post a reply please login or register