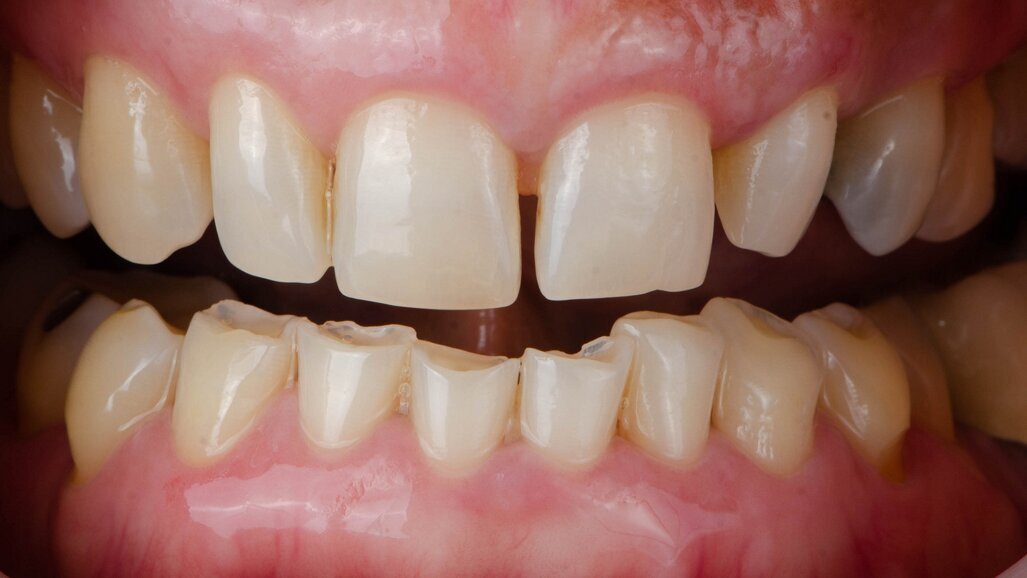
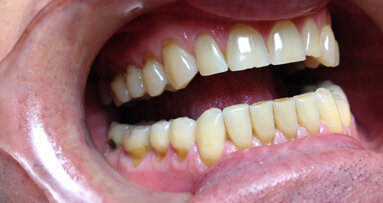
Bruxism-induced tooth wear gives rise to occlusal disease. Occlusal disease encompasses problems arising from abnormal or harmful contact between the maxillary and mandibular teeth. This includes joint and muscle problems, breakdown of dental restorations, and broader implications for overall health and well-being. The condition often affects one or possibly two components of the masticatory system, typically not all at once. If the temporomandibular joints are affected, it can lead to joint pain, difficulties in chewing and joint sound phenomena. Muscle involvement often results in headaches, myofascial pain and retro-orbital discomfort. Besides tooth wear, fillings and other restorations can break, and the periodontal ligaments can become stressed, leading to tooth mobility.
It may have further repercussions, depending on the way sufferers respond to these symptoms. For instance, this condition often leads to heightened tooth sensitivity, prompting a shift towards softer food choices. Consequently, individuals tend to consume foods rich in carbohydrates while avoiding tougher textures, like meats, which are more challenging to chew. This dietary adjustment can result in a notable reduction in protein and fibre intake, thereby potentially affecting overall body health. Such changes in eating patterns not only affect oral health but can also have far-reaching implications on the individual’s general well-being, both physical and psychological.
Prevention and treatment
Managing bruxism and occlusal disease requires a multifaceted strategy, having the primary aim of alleviating stress. In treatment terms, the first line of defence in managing bruxism is the use of occlusal splints. These devices, when correctly designed and used, can prevent further damage to the teeth and jaw. However, their effectiveness depends on factors like design, cost and patient compliance.
Understanding the theory behind splints is crucial, as some types can worsen the condition. For example, soft splints, which are generally the only option available on the National Health Service, can be helpful for some but detrimental for others, whereas hard acrylic, fully adjusted splints offer more predictable results.
When teeth are already damaged, restorative treatment becomes necessary. This can range from using composite materials for minor repairs to full reconstructions using ceramics or gold, the latter of which is particularly well accepted by older patients. The choice of material and technique must be tailored to each patient’s specific needs and circumstances. Restorative treatments also need to take into consideration the correct occlusal principles to ensure longevity of the restorations and health of the masticatory system.



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



































To post a reply please login or register