LONDON, England: Routine dental appointments may offer a practical opportunity to identify undiagnosed diabetes risk, according to new research from King’s College London. The study examined the use of chairside screening in a dental setting and suggests that rapid, non-fasting testing could help dental teams flag patients with possible prediabetes or diabetes and thereby support earlier intervention. Its findings strengthen the case for dental settings as a screening touchpoint while also prompting important questions about which patients are most appropriate to test.
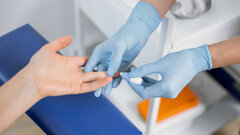
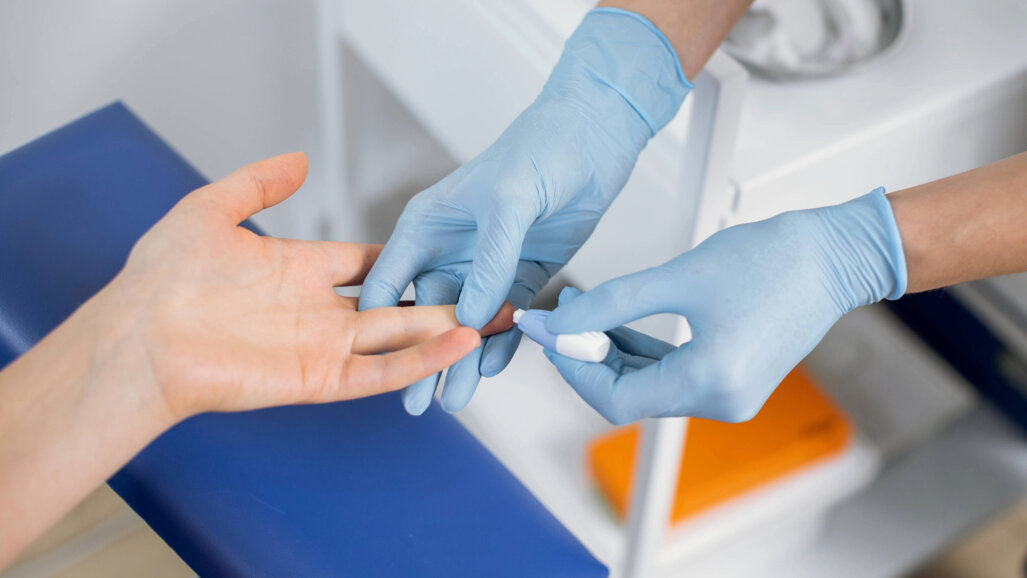
The study found that more than a third of dental patients with no prior diagnosis showed blood glucose levels consistent with prediabetes or diabetes when tested during routine appointments. The screening used a finger prick haemoglobin A1c (HbA1c) test, which measures average blood glucose over two to three months. Based on a cohort of more than 900 patients in a secondary care dental setting, the King’s study highlights that a significant burden of undiagnosed metabolic disease could be identified opportunistically in dental clinics.
The authors also examined whether periodontal status might help identify which dental patients are most appropriate for diabetes screening. They found that elevated HbA1c levels were associated with increasing severity of periodontal disease, but that relationship weakened once other factors were taken into account, suggesting that periodontal severity alone may be of limited value as an independent trigger for testing.
Clinically, the implications are considerable. Dental services provide access to patients who may not routinely attend primary care, offering an alternative pathway for early detection. The chairside test delivers results within minutes and does not require fasting, making it suitable for use during standard appointments. The findings indicate that the use of rapid HbA1c testing in this setting can provide a useful opportunity to identify previously unrecognised diabetes risk in order to enable timely referral for confirmatory diagnosis and management.
However, the researchers noted that the findings are based on a specific patient group with a high prevalence of periodontitis and that this may limit generalisability to other dental populations. Even so, the study underlines the potential for dental teams to contribute more actively to the early identification of chronic disease, supporting more integrated, preventive care.
Speaking on the significance of the study, lead author Dr Mark Ide, professor of periodontics at King’s, stated: “When the test reveals high levels of HbA1c, patients can then see their general medical practitioner to investigate further. This is something they might not have done without having the dental screening. Most of the patients in our study were surprised that they had elevated HbA1c levels and had no idea they might have prediabetes or diabetes.”
The importance of these findings is reinforced by recent UK research showing a lack of awareness among dental patients about the systemic link between periodontal disease and diabetes risk. In that context, the King’s study points not only to the screening potential of dental settings, but also to their possible role in improving awareness and promoting earlier medical follow-up. In that regard, the University of Birmingham’s INDICATE-2 study is now evaluating a dental care pathway in 50 high-street practices across the UK that involves diabetes risk assessment and finger prick HbA1c testing, followed by referral where appropriate.
The article, titled “Association between HbA1c chairside values and periodontitis”, was published online in the April 2026 issue of the Journal of Dentistry.
Topics:
Tags:
OSAKA, Japan: People living with Type 2 diabetes have been reported to experience a higher incidence of dental caries, but the biological pathways ...
LONDON, England: More than a third of UK adults in a study by periodontal health brand Corsodyl experience bleeding gingivae at least once a month when they...
LONDON, England: Although periapical periodontitis can increase systemic inflammation and is associated with cardiovascular risk and impaired glycaemic ...
FUKUOKA, Japan: World Diabetes Day, held annually on 14 November, highlights the need for greater awareness of the bidirectional relationship between ...
Live webinar
Thu. 9 April 2026
6:00 pm UTC (London)
Live webinar
Thu. 9 April 2026
7:00 pm UTC (London)
Prof. Moritz Kebschull, Cat Edney
Live webinar
Fri. 10 April 2026
3:00 pm UTC (London)
Live webinar
Fri. 10 April 2026
4:00 pm UTC (London)
Dr. med. dent. Henrik-Christian Carl Hollay
Live webinar
Fri. 10 April 2026
5:00 pm UTC (London)
Prof. Dr. Ali Murat Kökat
Live webinar
Fri. 10 April 2026
6:00 pm UTC (London)
Dr. medic. stom. Henriette Lerner
Live webinar
Fri. 10 April 2026
7:00 pm UTC (London)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East
































To post a reply please login or register