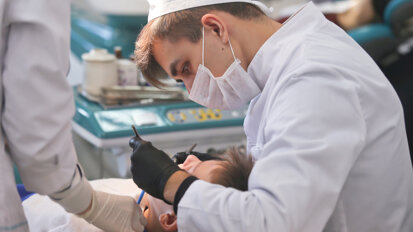
BIRMINGHAM, UK: To fill a research gap, researchers have recently examined whether dental professionals are, in fact, at an increased risk of becoming infected with SARS-CoV-2 in the workplace, as has often been hypothesised. They found that close contact with patients put dental professionals at a higher risk of developing COVID-19 during the first wave of the pandemic and that a large number of dental professionals had SARS-CoV-2 antibodies in their blood.
Just recently, Dental Tribune International (DTI) reported on a study that found that dentists from the US have successfully adopted the recommended infection control practices and have an extremely low SARS-CoV-2 infection rate compared with other front-line health professionals.
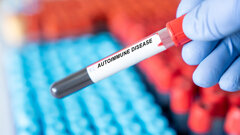
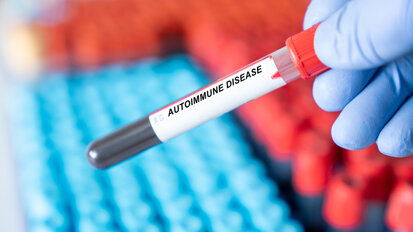
The present study involved 1,507 dental care practitioners from the West Midlands in the UK, including dentists, dental nurses and dental hygienists. To study the effect of dental professionals’ occupational exposure to the virus, the researchers took the participants’ blood samples at the start of the study in June 2020 and measured their levels of antibodies against SARS-CoV-2.
“Understanding what an antibody test result means to an individual with respect to their risk of infection is essential to controlling the pandemic,” first author Dr Adrian Shields, a clinical lecturer in the Institute of Immunology and Immunotherapy at the University of Birmingham, said in a press release. “Our study has taken the first steps in defining the level of antibody in a person’s blood necessary to protect them from infection for six months,” he continued.
“Our study has taken the first steps in defining the level of antibody in a person’s blood necessary to protect them from infection for six months”
— Dr Adrian Shields, University of Birmingham
The researchers found that, at the beginning of the study, 16.3% of the participants had SARS-CoV-2 antibodies, compared with only 6.0% of the general population at the time. The sample taken from dental practice receptionists, who have no direct patient contact, presented a low number of antibodies, comparable with that found in the general population. The finding supports the hypothesis that occupational risk is closely associated with patient exposure.
Additionally, the researchers found that ethnicity significantly increased the risk for infection. According to the data, 35.0% of Black participants and 18.8% of Asian participants had SARS-CoV-2 antibodies, compared with only 14.3% of white participants.
The second wave of the pandemic and SARS-CoV-2 immunity
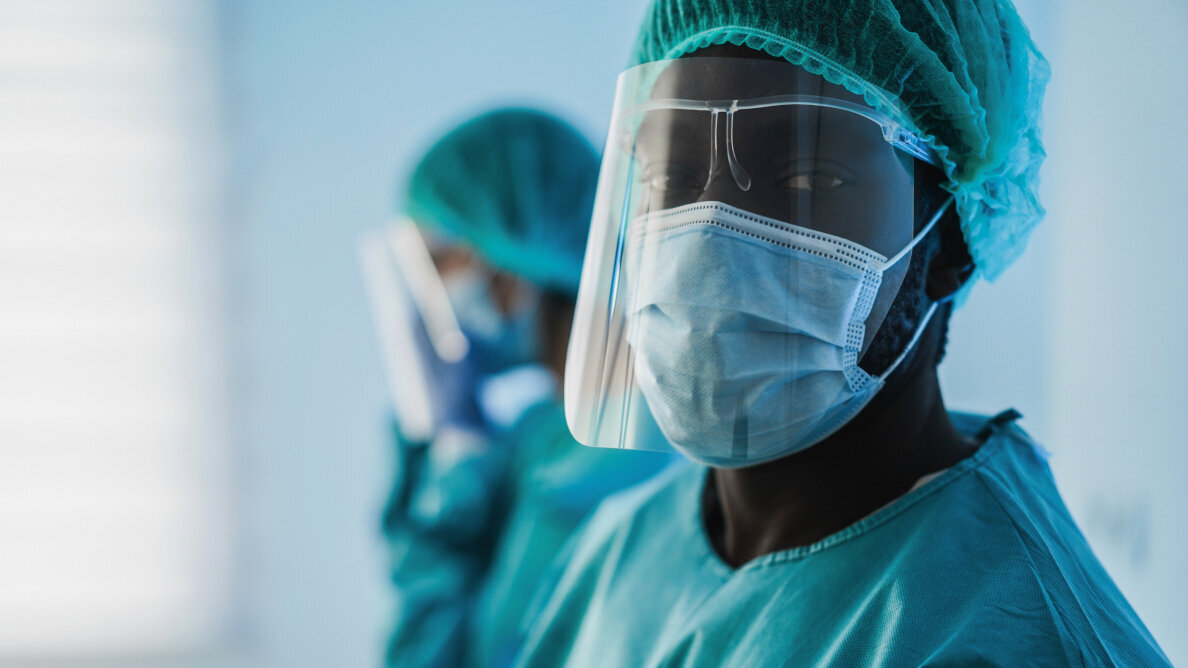
The researchers also took participants’ blood samples in September 2021, when dental practices in the UK had reopened, and then again in January 2021, six months after the baseline. During the period, healthcare workers were going through the second wave of the pandemic, and governments were rolling out vaccine plans. Needless to say, by that point, dental professionals had adopted strict infection prevention and control measures and clinicians had been provided with appropriate personal protective equipment (PPE), including face masks, face shields and gloves.
The results showed that, of those who had had previous COVID-19 infection, over 70% continued to have SARS-CoV-2 antibodies three and six months later. Additionally, the participants were found to be at a 75% reduced risk of reinfection with the virus. The study also examined the impact of COVID-19 vaccination. It reported that the vast majority of the participants without previous infection, 97.7%, developed an antibody response at least 12 days after receiving their first Pfizer vaccine, whereas participants who had previously been infected with the virus presented a more rapid antibody response that was higher in magnitude after a single dose of the vaccine.
DTI discussed SARS-CoV-2 reinfection and immunity at the beginning of the year and reported on a study that found that past infection may provide recovered COVID-19 patients with natural immunity which is effective for approximately half a year after the initial infection.
Finally, the researchers noted that none of the participants with a level of SARS-CoV-2 antibodies greater than 147.6 IU/ml in their blood had tested positive for COVID-19 during the period covered by the study. Co-author Dr Thomas Dietrich, professor of oral surgery at the university’s School of Dentistry, explained that only 5.3% of the cohort developed an antibody response that exceeded this threshold after the first wave of the pandemic in the UK and that this suggests that natural infection alone does not provide long-lasting immunity.
“Through our research, we have clearly shown that dental professionals were at increased occupational risk of exposure to SARS-CoV-2 prior to the new Public Health England guidance on PPE,” co-author Dr Iain Chapple, who is professor of periodontics at the university, stated in a press release.
“It is important that we now progress our research to ensure we have an understanding of how people are protected from reinfection with COVID-19 following natural infection and vaccination,” co-author Prof. Alex Richter, honorary consultant in clinical immunology at the university, added. “The nature and duration of immunity in these cohorts will be critical to understand as the COVID-19 pandemic progresses, particularly with respect to the efficacy of vaccination strategies—single-dose, multiple-doses, vaccine combinations—and in relation to novel viral variants of concern,” Richter concluded.
“It is important that we now progress our research to ensure we have an understanding of how people are protected from reinfection with COVID-19”
— Prof. Alex Richter, University of Birmingham
The study, titled “COVID-19: Seroprevalence and vaccine responses in UK dental care professionals”, was published online on 2 June 2021 in the Journal of Dental Research, ahead of inclusion in an issue.
Tags:



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



































To post a reply please login or register